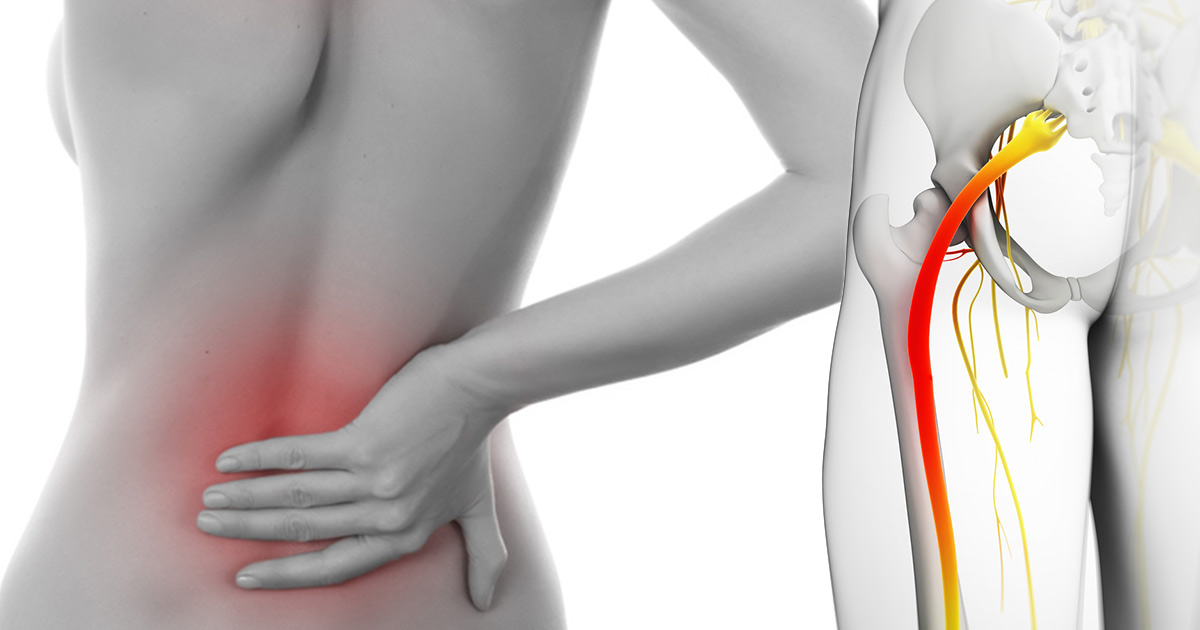
People, who are already suffering from sciatica nerve damage, will be well acquainted with the symptoms associated with it. When the sciatica nerve gets damaged, an individual would suffer from immense discomfort and pain, particularly when one pinches the area where the sciatic nerve is located. There are a lot of different things, which can be responsible for causing the pain. One can also experience diverse kinds of conditions, when he is suffering from sciatica. Not everybody encounters the same problems. Sciatic nerve damage can affect different areas.
Sciatic Nerve Damage Types
The most widespread problem that one faces owing to sciatica nerve damage is a herniated disk. This denotes that the disk becomes inflated. Again, it may begin to extend beyond its original position. These types of disks are created out of a substance, which is spongy in nature and they function as cushion between your spine and the vertebrae. Since the outer surface of these disks is made up of a shielding substance, they tend to have a hard exterior. When the outer surface of the disks gets damaged, it fails to provide protection to the disks, thus causing a lot of pain and discomfort to the patient.
Sciatica nerve damage can also be caused due to boney growths near your joints. Sometimes due to the wearing away of the bone cartilage, the bones start to rub against one another. Such a condition is known as bone spurs. Rubbing of bones against one another is a serious problem, since it can cause excessive pain. The area, which these bone spurs occupy is actually intended for the nerves. This kind of an occurrence can result in severe damage of sciatic nerve. This is one of the most widespread causes of sciatica nerve damage and it can be cured by means of many different techniques.
Sciatic Nerve Damage Results
Sciatic nerve damage affects individuals in various different ways. People can either suffer severely owing to a herniated disk or due to small bone spurs that become evident close to the joints.
The treatment for sciatica nerve damage generally includes exercises, proper rest and injections or medicines as prescribed. To get rid of the pain one can also try cold and hot compress. Doctors normally prescribe medicines based on the acuteness of the pain. The medicines that are most commonly prescribed for treating sciatica nerve damage are aspirin or ibuprofen. These medicines actually help to decrease the pain and inflammation. Cortisone injections and muscle relaxants are also found to be extremely effective for relieving severe pains.
Supplements like Nerve Renew, which are rich in minerals, are also prescribed by many doctors as a treatment for sciatic nerve damage. Doctors often recommend patients suffering from this condition to eat meals that are rich in magnesium and calcium. The intake of Vitamin B Complex supplements is also effective for treating sciatic. Regular intake of turmeric and ginger can also help to reduce the severity of this condition.
It has been found that yoga, acupuncture and acupressure can have a long-term effect on sciatic nerve damage. However, prior to beginning with these types of treatment, you need to find out whether or not your body will be able to accept these types of therapies. It is a common belief among people that acupuncture causes a lot of pain. However, in actual reality if it is performed by an expert, then it is absolutely painless and can produce effective results.
